The increasing tendency to recommend nonstress tests for high BMI in pregnancy has prompted many to ponder: Is this a necessary medical intervention or a suggestion rooted in weight bias?
In this article, we will dig into this big question, sift through the facts behind this recommendation, and provide questions you can ask your healthcare provider if you”re unsure whether this is the right choice for you.
Please note that while this article provides information on nonstress tests for high BMI (Body Mass Index), it should not be interpreted as medical advice. Every pregnancy is unique, and this information may not apply to your specific situation. Address any questions or concerns with your care provider.
The Nonstress Test, Explained
Nonstress tests (NSTs) rely on a specialized device called a cardiotocograph, commonly known as a fetal monitor, to provide antenatal fetal surveillance. The name “nonstress test” comes from the fact that the test is noninvasive and does not cause distress to the baby.
What is the purpose of a nonstress test?
Nonstress tests track the baby’s heartbeat from beat to beat, with the goal of seeing the heart rate go up and down from the baseline (more on that later). This offers a sneak peek into how the baby is doing inside the womb. The data from a nonstress test is analyzed on a paper printout or computer screen to look for potential signs of fetal distress.
How do nonstress tests work?
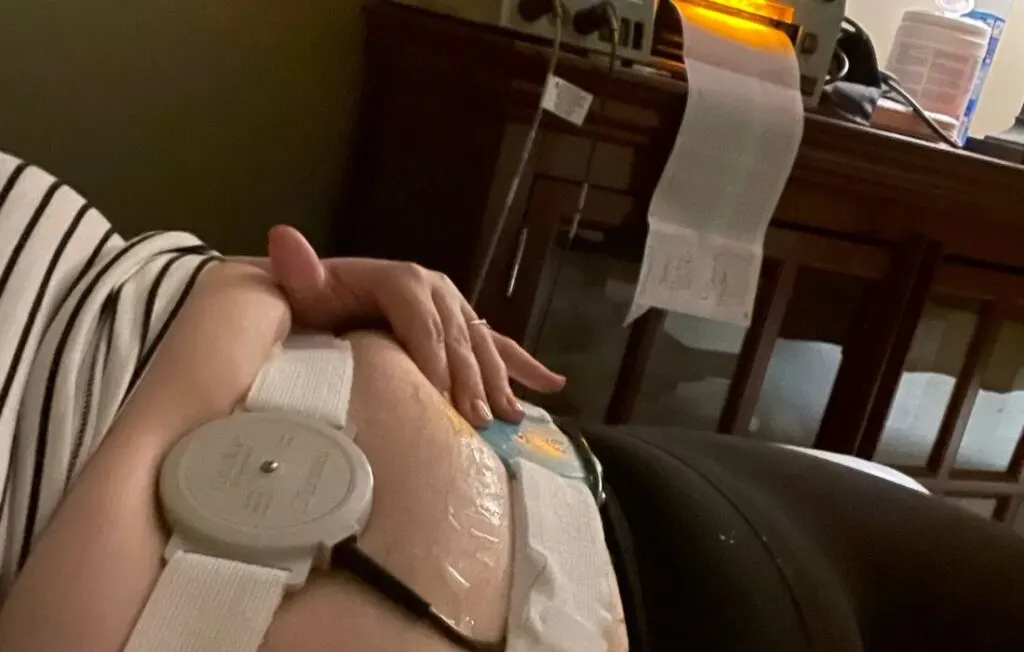
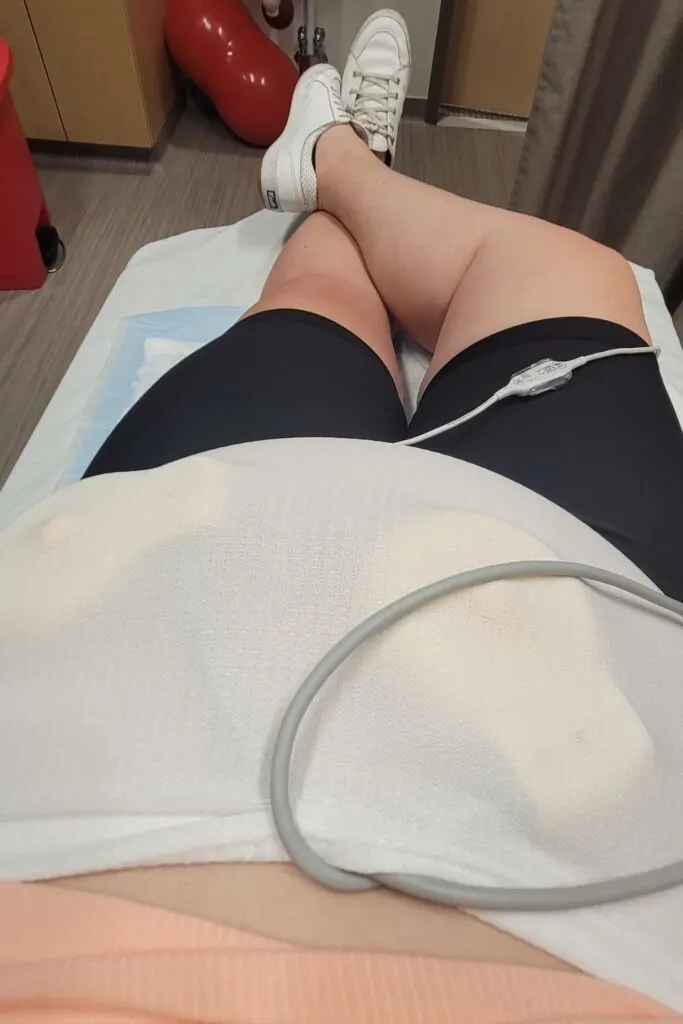
Two sensors are secured by belts on the person’s abdomen. One sensor catches even the faintest of contractions people might not notice. The other sensor tracks the baby’s heart rate. The NST lasts 20 to 30 minutes but sometimes up to an hour.
The person is typically in a semi-reclined or lying down position, sometimes on their left side, to promote blood flow. This position helps to keep them comfortable while the fetal monitor does its job. People should speak up if the belts are too tight or cause any discomfort.
Here’s a handy tip! If your facility doesn’t provide one, consider bringing a belly band for a nonstress test. These helpful accessories can ensure the monitors stay snugly in place. And here’s the best part – plus size belly bands are available!
What are the results of NSTs?
The NST is deemed “reactive” or reassuring when at least two instances of the baby’s heart rate speeding up, reaching a peak at least 15 beats per minute faster than the usual rate. Each of these speed-ups should last for a minimum of 15 seconds, starting from when it begins until it returns to the normal rate, all within a 20-minute window.
On the other hand, if these accelerations in the baby’s heart rate don’t happen within 40 minutes, the result is “nonreactive.”
A nonreactive NST does not necessarily mean there’s something wrong. The baby could be having a nap. Alternatively, it could suggest the need for additional testing, such as a biophysical profile, to gain a more comprehensive understanding of the baby’s health.
It’s important to note that NST can tell us how the baby is doing right at that moment, but it can’t predict what might happen in the future.
How well an NST works can depend on different things, including when the test is done, how active the baby is during the test, and how experienced the healthcare provider is at reading the test results. And it isn’t the only way doctors check a baby’s health.
When do nonstress tests happen during pregnancy?
Nonstress tests can be ordered at 26 to 28 weeks of pregnancy if the healthcare provider has concerns about the baby’s health. However, it is most commonly performed after 32 to 36 weeks when complications, including stillbirth, are more likely to occur.
Who are nonstress tests recommended for?
As we shared, having a nonstress test is for anyone if a healthcare provider has concerns about the baby.
With that said, weekly nonstress tests are relatively standard in high-risk pregnancies as part of the care plan nearing the end of pregnancy. This could include individuals with conditions such as gestational diabetes, high blood pressure, those carrying multiples, or advanced maternal age. In addition, nonstress tests for high BMI in pregnancy are a common suggestion.
The Costs of Nonstress Tests
An aspect we don’t often talk about when it comes to nonstress tests is what they truly cost – not just in money but also in terms of time spent and the possibility of causing extra worry.
We’ll start with time. Depending on the length of the test and waiting times, a single visit can eat into a good portion of someone’s day.
They may need to arrange childcare if they have children at home, adding potential expenses. Not to mention, the logistics of arranging for childcare can also cause stress.
Then, there’s the matter of potentially missing work, which could mean a loss of income.
Traveling to and from the healthcare provider’s office is another consideration. There’s the cost of gas or public transportation, and people need to factor in the price of parking, too.
These might seem like small details but they contribute to the added cost.
Additionally, the out-of-pocket costs can be considerable for some, depending on insurance coverage.
And let’s not forget the emotional impact, too. The knowledge that they are undergoing extra testing due to increased risk can generate anxiety and stress, which can negatively affect pregnancy outcomes.
On the flip side, NSTs can help alleviate stress! For instance, if someone is 40 weeks pregnant and the NST comes back with a reactive result, it could potentially provide more time for those who prefer to delay labor induction.
So, it’s important to consider all factors when discussing nonstress tests with healthcare providers.
Nonstress Tests for Plus Size Pregnancy
Now that we’ve covered what nonstress tests are and who should consider them, let’s turn our attention to the topic of nonstress tests in the context of high BMI during pregnancy.
Is a plus size pregnancy a high-risk pregnancy?
If someone has a BMI over 30, they are considered to have a plus size pregnancy.
More and more healthcare providers are categorizing plus size individuals as high-risk by default. However, this approach doesn’t align with the current guidelines set by the American College of Obstetricians and Gynecologists (ACOG), a leading authority in establishing standards for maternity care.
ACOG doesn’t explicitly state that a plus size pregnancy is high-risk. However, they do have recommendations for additional testing and oversight for people with a BMI over 30 during pregnancy.
Some people prefer the additional testing and oversight of a high-risk pregnancy; there’s nothing wrong with that. However, if someone is uncomfortable having a high-risk label based only on BMI and no other health concerns, it’s perfectly okay to consider finding a new care provider.
And if a healthcare provider always seems to link everything back to weight or makes fatphobic remarks, it’s worth trying to connect with a size-friendly care provider.
Weight bias in maternity care is a serious concern that can lead to substandard care and poor health outcomes. Advocating for yourself and seeking care from providers who approach your health from a comprehensive, individualized perspective is essential.
What are ACOG’s recommendations for nonstress tests for High BMI?
The main concern ACOG notes in their practice bulletin, number 230, which is unfortunately behind a paywall, is the increased risk of early fetal loss and stillbirth for people with a BMI over 35.
Therefore, ACOG states that weekly antenatal fetal surveillance may be considered starting at 37 weeks for anyone with a prepregnancy BMI between 35 and 39.9. Someone with a BMI of 40 or more may consider starting this surveillance at the 34th week of pregnancy.
It should be noted that ACOG’s recommendations range from well-supported scientific evidence (level A), limited or inconsistent evidence (level B) to mostly consensus and expert opinion (level C), with their fetal surveillance advice falling into the latter.
ACOG also acknowledges that the evidence that NSTs improve overall outcomes doesn’t exist.
UpToDate, trusted by medical professionals but also behind a paywall, states the following, “Although an obesity-associated increased risk for perinatal mortality that increases with gestational age has been reported, the mechanism is unclear, and the value of antenatal fetal surveillance with nonstress tests or biophysical profile scoring in this setting has not been studied. Therefore, we initiate antepartum fetal assessment for standard indications, not for obesity alone.”
Do all plus size people have nonstress tests at the end of pregnancy?
No, not everyone has nonstress tests based on BMI alone.
Some care providers look at various factors, including the person’s overall health, medical history, any complications during the pregnancy. As well as the health and development of the baby.
As we shared, research shows a correlation between a higher BMI and increased pregnancy risks, such as early fetal loss and stillbirth. This connection is a significant factor in why healthcare providers suggest NSTs as part of prenatal care. But remember that it’s a suggestion, not a requirement.
It’s essential to know that it’s a slightly increased risk of stillbirth, and knowing that the overall risk remains very low is crucial.
Also, knowing the difference between ‘absolute risk’ (the chance of something happening to you personally) and ‘relative risk’ (comparing risks between different people) is also reassuring. Sometimes, how statistics are shared can make things seem scarier than they are!
Speaking with your healthcare provider early in your prenatal care about your BMI and what specific recommendations they might have for your care can help set the stage for a healthy pregnancy journey.
So, while some plus size women have nonstress tests towards the end of their pregnancy, others will not. It’s a highly individual decision based on each pregnancy’s specific needs, made in consultation with healthcare providers providing informed consent.
How To Talk With Your Care Provider
Your emotional well-being is as important as your physical health during pregnancy. If you find that the recommendation for any procedures is causing significant anxiety, communicate this to your healthcare provider immediately!
Your care team can provide support, reassurances, and alternative approaches that can help ease your concerns while still looking out for your and your baby’s health.
It’s perfectly acceptable and advisable to ask questions about your care provider’s recommendations.
Why are they suggesting nonstress tests?
Is this recommendation based on your BMI alone, or are there other risk factors at play?
And importantly, what alternatives, if any, are available?
You have the right to understand the benefits and limitations of any tests, including nonstress tests. You also have the right to refuse any test you don’t want.
Below are some suggestions about how to talk to your care provider about nonstress tests for high BMI.
Ask About The Necessity
As the risk of stillbirth remains relatively low, you can discuss whether the tests are truly necessary. This discussion will help you make an informed decision about your care.
Express Your Concerns
Be candid about any anxiety or stress you may be experiencing due to the recommended testing regimen. Discuss the time and financial commitments.
Your healthcare provider might suggest resources or workarounds to help manage things better. They might also be able to provide reassurances, suggest coping mechanisms, or adjust your care plan.
Explore Alternatives
Ask if there are other ways to monitor your baby’s health that don’t require additional appointments.
Consider a Second Opinion
If you feel uncertain or uncomfortable about the recommended course of action or are concerned that your provider might have a weight bias, seeking a second opinion can be beneficial. Another healthcare provider may offer different insights or approaches that could resonate better with your personal situation.
Let’s loop back to the initial question about nonstress tests for high BMI.
While nonstress tests give us important information about fetal health, suggesting them as a standard procedure for pregnancies with a higher BMI certainly opens up a conversation worth having.
If your care provider suggests NSTs, it’s important to hear why they recommend these tests. Consider the time they take, how much they cost, and if they might make you feel stressed or anxious. Then have an open and honest conversation with your provider.
Ultimately, your emotional well-being, as well as your physical health, should be considered during your pregnancy.
Remember, you and your healthcare team have a shared goal – a healthy pregnancy and a healthy baby. So, how do you achieve this? By having frank, open discussions and asking all the questions you need to make decisions that are in the best interests of you and your baby.
Nonstress Tests For High BMI References
- Umana OD, Siccardi MA. Prenatal Nonstress Test. [Updated 2023 Feb 19]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan.
- Obesity in Pregnancy: ACOG Practice Bulletin, Number 230. Obstet Gynecol. 2021 Jun 1;137(6):e128-e144. doi: 10.1097/AOG.0000000000004395. PMID: 34011890.
- Aune D, Saugstad OD, Henriksen T, Tonstad S. Maternal body mass index and the risk of fetal death, stillbirth, and infant death: a systematic review and meta-analysis. JAMA. 2014 Apr 16;311(15):1536-46. doi: 10.1001/jama.2014.2269. PMID: 24737366.


